Why Some Eczema Patients Worsen with Moisturizers?

What’s Inside?
- What is eczema?
- Types of Eczema
- Common Causes/Triggers of Eczema
- Pharmacological and non-pharmacological treatments
- What are the moisturizers?
- Types of moisturizers
- Answer to the question that why some eczema patients worsen with moisturizers?
- Right way of using moisturizers
- General adverse effects of moisturizers
Eczema:
Eczema is a term used to represents a group of inflammatory skin conditions which involves skin dryness, redness, itchiness, rashes, blisters, and skin patches which all can also progress to skin infections. Though the eczema in not curable but the symptoms can be managed using various medications.
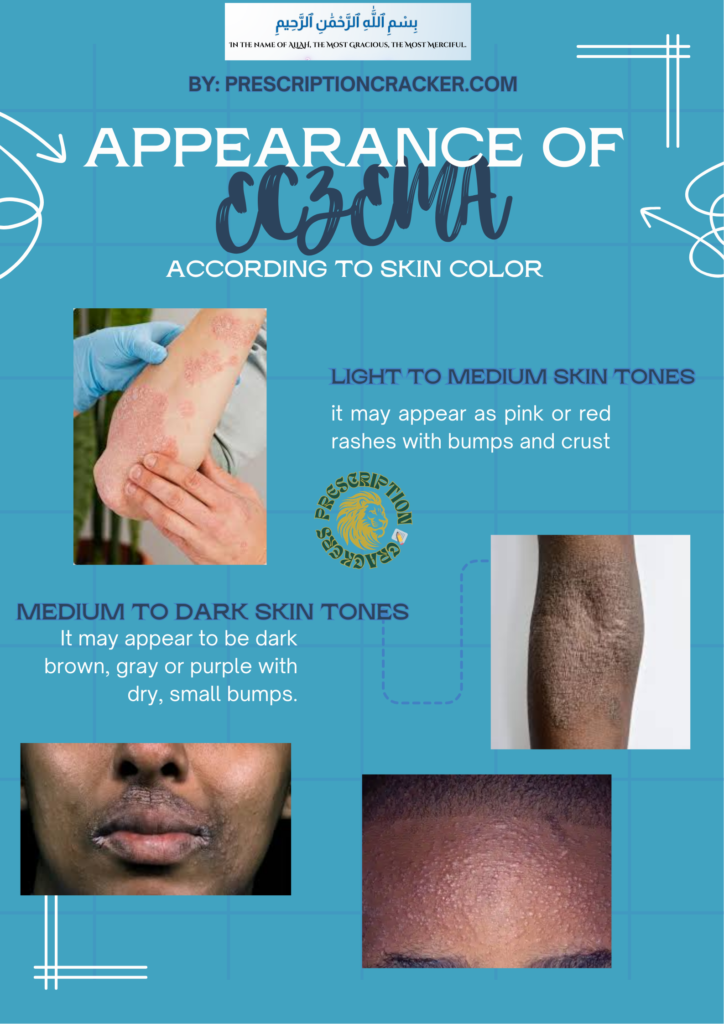
The manifesting signs of eczema vary from to person and from skin to skin. Here’s how it shows its signs according to the patient’s skin:
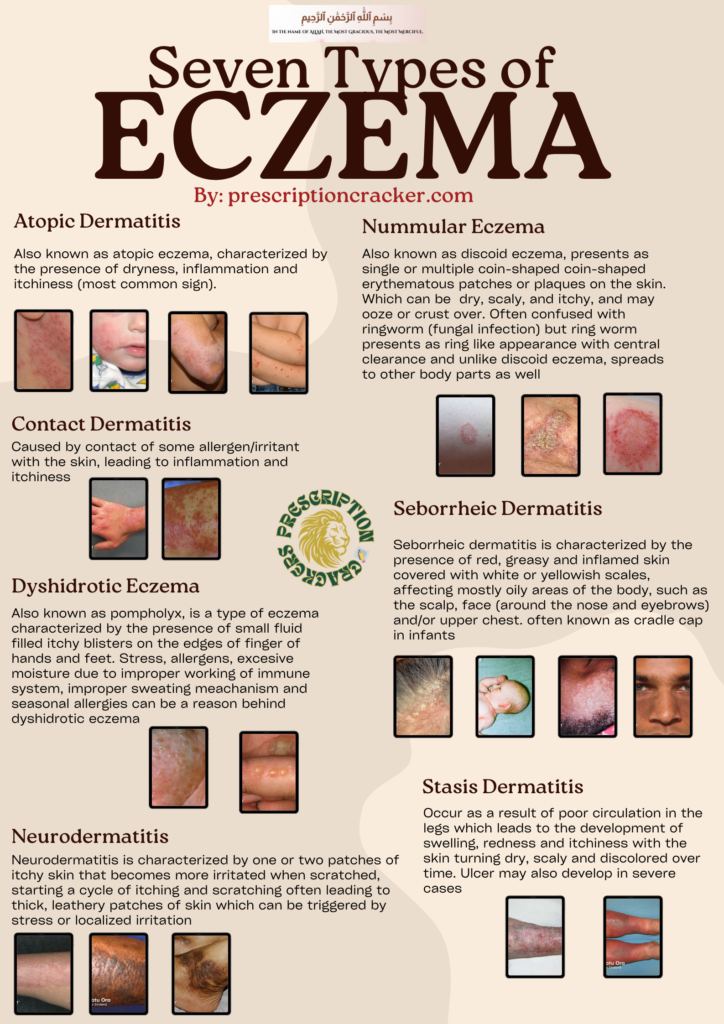
Seven types of eczema:
Seven types of eczema have been identified in the humans that affects the skin. Some of them share overlapping manifesting signs while other can be differentiated easily. These includes:
- Atopic Dermatitis (atopic eczema)
- Contact dermatitis
- Dyshidrotic eczema (pompholyx)
- Neurodermatitis
- Nummular eczema (discoid eczema)
- Seborrheic dermatitis (cradle cap in infants)
- Static dermatitis
Common Causes or triggers of Eczema:
There are a number of factors or triggers that could be attributed to the occurrence of eczema. Some of most common factors includes:
- Family History/genetics
- Over reactive immune system
- Weakened skin barrier
- Stress
- Food allergens such as egg, peanuts, milk, fish, soy, rice, and wheat.
- Environmental triggers
Among the environmental triggers following factors are considered to be the most important:
Fabrics:
Fabrics comes in direct contact with the body so is considered to be one of the most important triggers of eczema in sensitive individuals. Some of the most important fabric materials that are identified to be involved in the initiation of eczema attack particularly contact dermatitis, includes the following:
- Wool
- Latex (e.g. in gloves, condoms, clothes, ballons, mattresses, paints, adhesives, toys, shoe soles, baby bottle nipples and pacifiers, diapers, sanitary napkins, and other pads and elastic etc.)
- Synthetic fabrics (e.g. polyester, nylon, acrylic and fleece etc.)
Metals:
Some of the metals can trigger the eczema attack in some individuals. These includes:
Cobalt/Cobalt Chloride: Mostly industry workers came across Cobalt chloride while working. Other people may come across it through various products like it is found in:
- Jewellery
- Cosmetics e.g. blushers, eye shadows and compact powder etc.
- Hair dyes
- Leather
- Dental alloys
- Paints
- Ceramics
- Blue tattoo pigments
- Animal feeds
- Printing inks
- Vitamin B12 tablets and injections.
Chromium Allergy:
Chromium is found in various products of daily use such as:
- Yellow or green colored cosmetics
- Green fabric that is used to cover snooker or card tables
- Green or yellow ink used for making tattoos
- Radiator coolants
- Orthopaedic or dental implants
- Chrome tanned gloves, shoes or other stuff
Nickel Allergy:
Nickel is one the most important metal that is found in a number of materials like:
Jeweller: necklaces, necklace-clips, earrings, bracelets, watch-straps and rings, may contain nickel.
“If a person is allergic to nickel, then he/she can use hypoallergenic stainless steel, solid gold (12 carat or more), or silver jewellery. Nickel is found in 9-carat gold and white gold. Plastic covers for earring studs can be used. Coating the stud with nail varnish is not recommended as the varnish could soon chips off leaving the nickel in direct contact with skin.
Clothing Material: Nickel is widely used in clothing such as jean’s buttons, metal zips, bra hooks, hair pins, and studs etc. Plastic or paint coated metals are safe to use in people with nickel allergy.
Nickel containing Household items:
- Knives
- Pens
- Razors
- Keys
- Rings
- Mobile phones
- Lipstick holders
- Handbag catches
- Cupboard handles
- Kitchen utensils
- Bath plugs
- Vacuum cleaner
- Scissors
- Needles
- Toaster
- Coins (money): Cashiers should use gloves
Nickel Containing Office item:
- Paper clips
- Typewriter Keys
- Other metal Instruments
Nickel Containing Foods: Any fruit, dry fruit, nuts, vegetables, spaghetti or any drink that is present in “can” should also be avoided in patients with nickel allergy.
Some people are also allergic to gold and copper (found in electrical wires, coins, plumbing pipes, jewellery, and household utensils).
Other environmental triggers include:
- Pets and insects: Pet dander, cockroaches, insect bites and stings
- Weather e.g.Temperature and seasons variations, humidity, extreme heat or cold
- Stress e.g.Life stressors, and anxiety
- Environment e.g.Pollen, dust mites, Mold, cigarette smoke
- Fragrance e.g.Perfumes, other scented products
Pharmacological and non-pharmacological treatments of Eczema patients:
- Identification and prevention of triggers of eczema.
- Adequate Hydration.
- Daily moisturization particularly after taking bath to lock the moisture in the skin, often known as soak and smear technique (preference is given to, fragrance and preservatives free, ointments over creams due to low water content).
- Antihistamines can be used for excessive itching associated with eczema and halting the further progression of allergic reactions especially in case of insect bite.
- Diluted bleach baths or intranasal mupirocin is recommended in patients with poorly controlled eczema for the prevention of cutaneous infections.
- Topical anti-inflammatory medications such as topical steroids or steroid-free products like pimecrolimus, or tacrolimus.
Topical steroids should only be used for the active lesions or prophylactically few times a week for the prevention of flare-up of eczema. Topical steroids should not be recommended for the long-term usage due to the potential risk of adverse effects.
- Other FDA approved medication includes: crisaborole (EUCRISA®) for children >3 months of age and older and with mild to moderate eczema, and Dupilumab (S/c injection) which is used to treat adults and children 6 months of age and older with moderate-to-severe eczema that is not well controlled with topical prescription therapies, or who cannot use topical therapies.
Complications of Eczema Patients:
- Bacterial infection can occur upon eczema lesions.
- Viral infections such as Eczema herpeticum caused by herpes simplex virus-1 and eczema cosackium.
Moisturizers:
Moisturizers are the topical products used to enhance moisture in the skin while emollients are the topical products that are employed to soften and smooth the skin surface. Though both the terms emollient and moisturiser are often used interchangeably, emollients can also be regarded as a specific ingredient of moisturisers.
There are various types of moisturizers available in the market containing different ingredients that adopt diverse mechanisms for the bringing the effect of moisturization to the skin. Some of the most commonly used moisturizers and their mechanism are mentioned below:
Types of Moisturizers and their mechanism of action:

Another important type of moisturizer includes protein rejuvenators that are the small molecular weight proteins, used rejuvenate the skin by replenishing skin’s essential proteins. These includes collagen, elastin, keratin.
The moisturizers are formulated in various ways, mostly using humectant, occlusives and emollients in different proportions. Such as Occlusives and humectants are mostly combine to enhance the skin’s water-holding capacity. Addition of some emollients may improve the aesthetic quality and stability of moisturizer’s active ingredients. The most common formulation is cosmetic emulsions, most are lotions (oil-in-water emulsions) or creams (water-in-oil emulsions). Complex emulsions (e.g., oil-in-water-in-oil, oleaginous mixtures, serums, gels, sprays, and milks) are used to deliver and stabilize some active ingredients.
Why Some Eczema Patients Worsen with Moisturizers?
As we know that there are various types of moisturizers that can be used for various skin conditions including eczema/dermatitis, one of the most important moisturizers that used to be applied in past for the management of eczema but with the passage of time, response of the patient and research studies they were found to be associated with the worsening of eczema. These are aqueous creams BP.
Aquoeus creams BP is not considered really effective due to poor moisturizing effect. Apart from this it also contains an ingredient name as “sodium lauryl sulphate (SLS)”, which have the potential to irritate the skin and make the eczema worse. Several emollients have been reformulated in recent years to remove SLS.
The skin has a protective barrier layer made up of lipids, approximately one eighth the thickness of a sheet of paper, that prevent chemicals from getting inside the body and keeps moisture lock in the skin.
Sodium lauryl sulphate (SLS) is a detergent that is used to mix oils into water-based moisturisation creams to give a good creamy texture. It’s also used extensively in shower gels and other cosmetics.
It has been found by research studies that rubbing aqueous cream containing SLS upon the skin causes the thinning of protective barrier of the skin, making the skin more susceptible to irritation by chemicals.
Thus, using aqueous creams BP on eczematous skin, which is already thin and vulnerable to irritation, is likely to make the condition even worse.”
Studies have recommended that it is better to use oil-based ointments on the damage skin of eczema patients rather than aqueous creams BP.
“SLS is an ingredient that should never be included in an emollient formulation”
Right Method of using a Moisturizer:
Application of the moisturizer in the correct way is the key to get optimal response from it. Thus, following measures should be kept in mind to get maximum benefit from a moisturizer:
- Emollient base moisturizers should be applied on the moist skin. Applying the emollient base moisturizer after shower or sponge bath, in the direction of hair follicles, gives excellent moisturizing effect.
- Never rub the moisturizer up and down on the skin, always apply it in the direction of hair follicles, as this could trigger itchiness, block hair follicles and can cause inflammation.
- The moisturizer should be applied all over the skin, not just upon the eczema affect areas.
- The moisturizer should be continued even after the resolution of the symptoms in order to prevent future flare ups.
- When steroidal creams/ointments are also suggested by the dermatologist, then first apply the steroidal cream/ointment, wait for 30 minutes and then apply the moisturizers especially those that contains occlusives or emollients in order to avoid the dilution and hinderance of absorption of steroidal cream/ointment.
- In case of calcineurin inhibitors (tacrolimus) base topical creams/ointments, the gap between the application of moisturizer should be at least 2 hours. This means using emollients and/or soap substitutes, and then leaving a 2-hour gap before applying tacrolimus base.
General Adverse effects of moisturizers:
Adverse Effect | Possible Causes |
Subjective irritation | Humectants (lactic acid, urea); preservatives such as benzoic acid or sorbic acid |
Irritant reactions | Proteins in vegetable oils, urea, hydroxyl acids, propylene glycols, solvents |
Allergic contact dermatitis | Lanolin; propylene glycols; vitamin E, Kathon CG, preservatives, fragrances, sunscreens, herbal ingredients (tea tree oil, olive oil, chamomile oil, aloe) |
Occlusive folliculitis | Petrolatum & mineral oils |
Photosensitivity eruptions and photo melanosis | Fragrances, hydroxyl acids, preservatives, sunscreens |
Cosmetic acne | Occlusive oils used in water-in-oil preparations |
Contact urticaria | Preservatives such as sorbic acid, fragrances, & balsam of Peru |
Poisoning in burn patients | Propylene glycol |
Intoxication | Salicylic acid |
References:
National Eczema Association. (n.d.). Eczema. National Eczema Association. https://nationaleczema.org/eczema/
Everyday Health. (n.d.). What to do when atopic dermatitis causes dark patches or light spots on skin. Everyday Health. https://www.everydayhealth.com/eczema/what-to-do-when-atopic-dermatitis-causes-dark-patches-or-light-spots-on-skin/
WebMD. (2024, March 11). How eczema affects darker skin tones. WebMD. https://www.webmd.com/skin-problems-and-treatments/eczema/eczema-darker-skin-tones
SkinSight. (n.d.). Atopic dermatitis (eczema). https://skinsight.com/skin-conditions/atopic-dermatitis-eczema/child/ (Accessed 2026).
Neodermatologist. (n.d.). Nummular eczema vs. ringworm. https://www.neodermatologist.com/blogs/nummular-eczema-vs-ringworm (Accessed 2026).
DermNet NZ. (n.d.). DermNet NZ. https://dermnetnz.org/ (Accessed 2026).
MedlinePlus. (n.d.). Patient instructions for eczema care. U.S. National Library of Medicine. https://medlineplus.gov/ency/patientinstructions/000500.htm (Accessed 2026).
DermNet NZ. (n.d.). Allergy to cobalt. https://dermnetnz.org/topics/allergy-to-cobalt (Accessed 2026).
DermNet NZ. (n.d.). Chrome allergy. https://dermnetnz.org/topics/chrome-allergy (Accessed 2026).
DermNet NZ. (n.d.). Jewellery allergy. https://dermnetnz.org/topics/jewellery-allergy (Accessed 2026).
National Center for Biotechnology Information. (n.d.). In StatPearls. https://www.ncbi.nlm.nih.gov/books/NBK538209/ (Accessed 2026).
Asthma and Allergy Foundation of America. (n.d.). Skin allergies and eczema. https://acaai.org/allergies/allergic-conditions/skin-allergy/eczema/ (Accessed 2026).
National Eczema Society. (n.d.). Emollients and eczema. https://eczema.org/information-and-advice/treatments-for-eczema/emollients/ (Accessed 2026).
Nursing Times. (2010, October 20). Eczema made worse by aqueous cream. Nursing Times. https://www.nursingtimes.net/dermatology/eczema-made-worse-by-aqueous-cream-20-10-2010/ (Accessed 2026).
ScienceDaily. (2010, October 18). Findings on eczema and aqueous cream. https://www.sciencedaily.com/releases/2010/10/101018074536.htm (Accessed 2026).
Pittelkow, M. R., & Soter, N. A. (2018). Eczema and contact dermatitis: Clinical insights. In StatPearls. National Library of Medicine. https://pmc.ncbi.nlm.nih.gov/articles/PMC5849435/
Research Articles, Case Studies & Pharma Bulletin
Disclaimer
This article is for informational and educational purposes only. It does not substitute for professional medical advice, diagnosis, or treatment. Always consult a qualified healthcare provider before starting any medication.