Why does CRP increases but ESR stay normal?

C-reactive protein (CRP):
C-reactive protein (CRP) is a protein that is produced in the liver by hepatocytes. The level of CRP increases during the period of inflammation especially during acute inflammation. These proteins are released by white blood cells during inflammation. CRP is considered as an important acute phase reactant.
FAQ: What is Acute phase reactant?
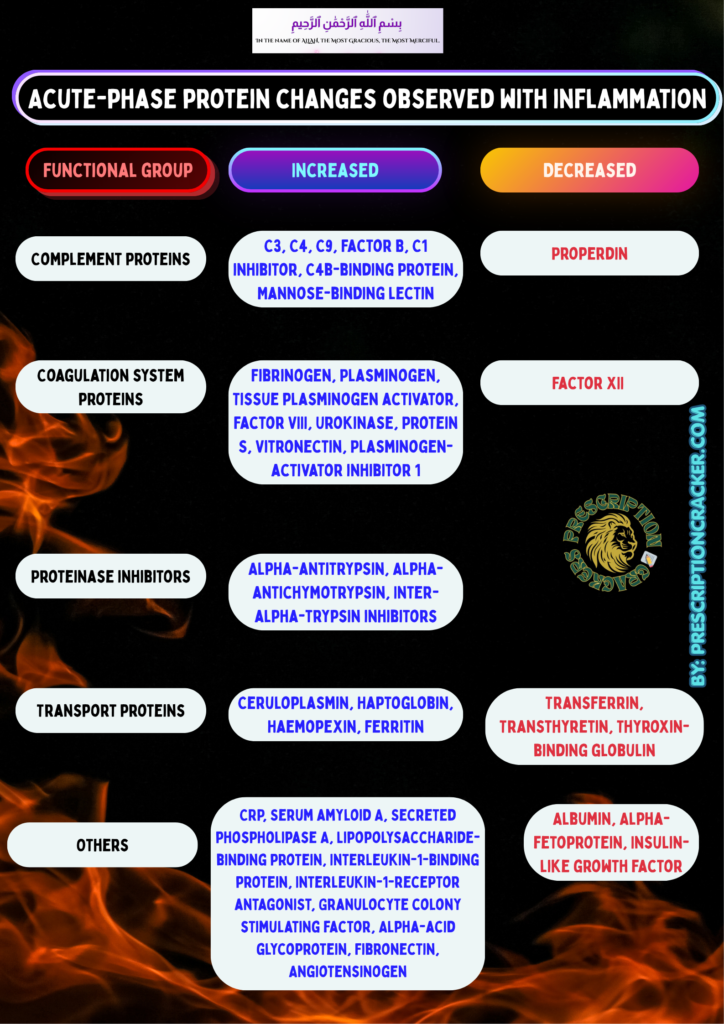
Acute phase reactants are the proteins whose level in the blood decreases or increases by almost 25% or more during the inflammation in the body. There are many acute phase reactants that increases or decreases as a response to inflammation. Some of them are mentioned in the image below:
Conditions where CRP is routinely measured:
The Conditions in which C-reactive protein test is recommended includes the following:
Assessment of disease activity of autoimmune/ autoinflammatory conditions:
- Rheumatoid arthritis
- Juvenile idiopathic arthritis
- Seronegative arthritis
- Ankylosing spondylitis
- Reactive arthritis
- Psoriatic arthritis
- Crohn’s disease
- Rheumatic fever
- Vasculitis
- Behcet’s syndrome
- ANCA-associated vasculitis
- Polyarteritis nodosa
- Pancreatitis
- Periodic fever syndromes
Assistance with diagnosis and monitoring of infection:
- Bacterial endocarditis
- Abscess
- Postoperative infection
- Response to antibiotic therapy
Differentiation between inflammatory conditions:
- Systemic lupus erythematosus vs rheumatoid arthritis (CRP is almost absent during SLE, most probably due to the presence of IFN-alpha, which is up-regulated in SLE and inhibits CRP)
- Crohn’s disease vs ulcerative colitis (CRP shows no or mild elevation in ulcerative colitis)

Erythrocytes Sedimentation Rate (ESR):
The erythrocyte sedimentation rate (ESR) test is defined as test in which the time taken by red blood cells to settle at the bottom of the tube, is measured. ESR test is used for the detection of the inflammation in the body as during the inflammation the level of blood proteins increases such as fibrinogen (most prominent), beta-globulins, alpha-globulins, gamma-globulins and albumin (less prominent).
High level of blood protein (particularly fibrinogen, accounts for 60-70% of the increase in ESR) promotes the aggregation of red blood cell which cause them to settle rapidly at the bottom of the tube.

Other Reasons for increase in ESR:
Female usually have slightly higher ESR values than the male patients. Pregnancy and advancing age are also linked to increased ESR. Other contributing factors includes anemia, RBC abnormalities, and procedure errors such as: tilted ESR tubes, elevated specimen temperature, and dilution errors.
Why does CRP increase but ESR stay normal?
It has been observed that both CRP and ESR are used as the indicators of inflammation. But it is often observed that while CRP is increase, ESR remains normal during the test. The answer to this question lies in time of the testing after the appearance of symptoms.
In the first 24 hours of a disease process, the CRP is rapidly elevated while the ESR mostly remains normal. When the source of inflammation is removed, the C-reactive protein will return to its normal state, almost within a day or two. However, the ESR will remain elevated for several days until excess fibrinogen is removed from the serum.
ESR have long half-lives, it is less worthy for the assessment of acute changes than CRP. An elevated ESR may be due to events that have occurred many weeks or months back and may have resolved at the time of measurement.
So, this is the reason why, when the patient is tested for CRP and ESR during the first 24 hours of the disease process, the level of CRP comes out to be elevated while the values of ESR remains normal.
It is also noteworthy that in osteoarthritis, ESR is usually remains normal while CRP may get elevated. The level of C-reactive protein, in osteoarthritis, is used as a predictive biomarker for the severity and duration of the disease.
One very important thing to mention is that the elevated level of ESR and CRP also signs toward the presence of an infection in the body, so neither test can be adopted as an absolute diagnostic tool for the existence of the inflammation or pain.
References:
Australasian Association for Clinical Biochemistry and Laboratory Medicine. (n.d.). Making sense of inflammatory markers. Royal College of Pathologists of Australasia.
https://www.rcpa.edu.au/getattachment/13421292-28ae-4a1d-bdb4-3c91c073d7f2/Making-Sense-of-Inflammatory-Markers.aspx
StatPearls Publishing. (2024). C-reactive protein. In StatPearls. National Center for Biotechnology Information.
https://www.ncbi.nlm.nih.gov/books/NBK441843/
MedlinePlus. (2024). Erythrocyte sedimentation rate (ESR). U.S. National Library of Medicine.
https://medlineplus.gov/lab-tests/erythrocyte-sedimentation-rate-esr/
Tishkowski, K., & Zubair, M. (2025). Erythrocyte sedimentation rate. In StatPearls. StatPearls Publishing.
https://www.ncbi.nlm.nih.gov/books/NBK557485/
University of Rochester Medical Center. (n.d.). C-reactive protein (serum). Health Encyclopedia.
https://www.urmc.rochester.edu/encyclopedia/content?contentid=c_reactive_protein_serum&contenttypeid=167
American Academy of Family Physicians. (n.d.). Don’t order an erythrocyte sedimentation rate to look for inflammation in patients with undiagnosed conditions. Choosing Wisely.
https://www.aafp.org/pubs/afp/collections/choosing-wisely/243.html
Pharma Bulletin, Research Articles & Case Studies
Disclaimer
This article is for informational and educational purposes only. It does not substitute for professional medical advice, diagnosis, or treatment. Always consult a qualified healthcare provider before starting any medication.